All The Things You Want To Know On The Subject Of Pain In The Arches
Overview
The phrase arch pain (or arch strain) refers to an inflammation and/or burning sensation under the long arch of the foot. This is a common foot condition that can be easily treated. Arch pain (arch strain) has the tendency to occur as a result of overuse in activities / exercises such as running, jumping, tennis, squash, hiking, walking, and skiing / snowboarding. People who have flat feet, or people whose feet flatten and roll inward (called ?over pronation?) are more prone to arch pain. Arch pain usually occurs gradually. However, it can occur suddenly if the fascia ligaments are stretched or torn during a forceful activity such as sprinting or jumping. An accurate diagnosis from a podiatrist (foot doctor) is important early in the management of arch pain.
Causes
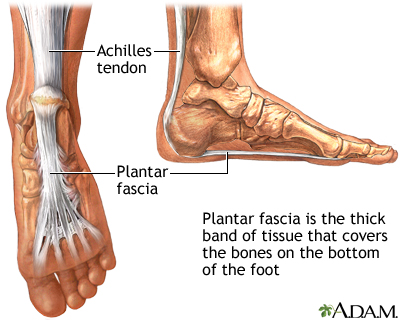
Plantar fasciitis, another sports injury detailed on this website, is regularly the cause of foot arch pain or strain. This can arise due to faulty biomechanics in your feet, which alone can also provoke foot arch pains. The most prominent biomechanical difficulties are flat feet and high arches. With flat feet (or overpronation) the arches appear to be almost flattened, causing unevenness by forcing the feet roll inwards in order to maintain balance and support the body's weight. This places inordinate pressure on the plantar fascia and arches. If by contrast you have high arches (instep), the ankle can roll outwards, again causing undue strain on the arches. Too much of this strain can lead to stretching of the plantar fascia and pain in the arches. Other causes include overstretching or otherwise pressuring the arches, for example by exercising with fatigued leg muscles which leave the feet with excessive work to do. You are also particularly at risk if in your 40s or 50s and commencing an intense program of training after a long period of inactivity.
Symptoms
Most flat feet do not cause pain or other problems. Children may have foot pain, ankle pain, or lower leg pain. They should be evaluated by a health care provider if this occurs. Symptoms in adults may include tired or achy feet after long periods of standing or playing sports.
Diagnosis
The medical practitioner will examine how the muscles of your foot function. These tests may involve holding or moving your foot and ankle against resistance; you may also asked to stand, walk, or even run. Pain caused by movements may indicate the cause of the pain. The nerves in the foot will be tested to make sure no injury has occurred there. An x-ray, MRI, or bone scan of the foot and arch may be taken to determine if there are changes in the makeup of the bone.
Non Surgical Treatment
More than 90% of patients with plantar fasciitis will improve within 10 months of starting simple treatment methods. Rest. Decreasing or even stopping the activities that make the pain worse is the first step in reducing the pain. You may need to stop athletic activities where your feet pound on hard surfaces (for example, running or step aerobics). Ice. Rolling your foot over a cold water bottle or ice for 20 minutes is effective. This can be done 3 to 4 times a day. Nonsteroidal anti-inflammatory medication. Drugs such as ibuprofen or naproxen reduce pain and inflammation. Using the medication for more than 1 month should be reviewed with your primary care doctor. Exercise. Plantar fasciitis is aggravated by tight muscles in your feet and calves. Stretching your calves and plantar fascia is the most effective way to relieve the pain that comes with this condition.

Surgical Treatment
Foot surgery is difficult, especially when large amounts of deformity correction are needed. The ability to bring the foot into a new position may not be lasting, even if everything looks perfect in the operating room. The goal is to provide improved position and function of the foot and ankle. In some patients with very severe deformity, the goal is a foot that functions well in a brace. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Particular complications associated with cavus foot surgery include incomplete correction of deformity, return of deformity and incomplete fusion.
Prevention
So how do you prevent plantar fasciitis? Factors which can be controlled include training progression, environmental factors, shoes, and strength and flexibility exercises. A useful guideline for a safe training progression is ?the 10% rule.? Limit increases in distance or intensity to 10% a week. For example, if a person is running 60 minutes at a session, 4 times a week, or 240 minutes, she or he can probably increase the running time to 264 minutes (240 + 10%), the following week if all else remains the same. Terrain is also an important factor in training. Running 30 minutes on hills is very different from running 30 minutes on flat surfaces in terms of the forces on the legs and feet. Work up gradually to increase your running time on hills. Also lean forward when running downhill. If you run on a banked or crowned surface, vary the direction you run in so you alternate which leg is higher and which leg is lower on the bank. If you know concrete or asphalt is causing you discomfort, try running on a cinder or composite track. If you are going on vacation and are not used to running on sand or grass, don?t spend your whole vacation doing it.
The phrase arch pain (or arch strain) refers to an inflammation and/or burning sensation under the long arch of the foot. This is a common foot condition that can be easily treated. Arch pain (arch strain) has the tendency to occur as a result of overuse in activities / exercises such as running, jumping, tennis, squash, hiking, walking, and skiing / snowboarding. People who have flat feet, or people whose feet flatten and roll inward (called ?over pronation?) are more prone to arch pain. Arch pain usually occurs gradually. However, it can occur suddenly if the fascia ligaments are stretched or torn during a forceful activity such as sprinting or jumping. An accurate diagnosis from a podiatrist (foot doctor) is important early in the management of arch pain.

Causes
Plantar fasciitis, another sports injury detailed on this website, is regularly the cause of foot arch pain or strain. This can arise due to faulty biomechanics in your feet, which alone can also provoke foot arch pains. The most prominent biomechanical difficulties are flat feet and high arches. With flat feet (or overpronation) the arches appear to be almost flattened, causing unevenness by forcing the feet roll inwards in order to maintain balance and support the body's weight. This places inordinate pressure on the plantar fascia and arches. If by contrast you have high arches (instep), the ankle can roll outwards, again causing undue strain on the arches. Too much of this strain can lead to stretching of the plantar fascia and pain in the arches. Other causes include overstretching or otherwise pressuring the arches, for example by exercising with fatigued leg muscles which leave the feet with excessive work to do. You are also particularly at risk if in your 40s or 50s and commencing an intense program of training after a long period of inactivity.
Symptoms
Most flat feet do not cause pain or other problems. Children may have foot pain, ankle pain, or lower leg pain. They should be evaluated by a health care provider if this occurs. Symptoms in adults may include tired or achy feet after long periods of standing or playing sports.
Diagnosis
The medical practitioner will examine how the muscles of your foot function. These tests may involve holding or moving your foot and ankle against resistance; you may also asked to stand, walk, or even run. Pain caused by movements may indicate the cause of the pain. The nerves in the foot will be tested to make sure no injury has occurred there. An x-ray, MRI, or bone scan of the foot and arch may be taken to determine if there are changes in the makeup of the bone.
Non Surgical Treatment
More than 90% of patients with plantar fasciitis will improve within 10 months of starting simple treatment methods. Rest. Decreasing or even stopping the activities that make the pain worse is the first step in reducing the pain. You may need to stop athletic activities where your feet pound on hard surfaces (for example, running or step aerobics). Ice. Rolling your foot over a cold water bottle or ice for 20 minutes is effective. This can be done 3 to 4 times a day. Nonsteroidal anti-inflammatory medication. Drugs such as ibuprofen or naproxen reduce pain and inflammation. Using the medication for more than 1 month should be reviewed with your primary care doctor. Exercise. Plantar fasciitis is aggravated by tight muscles in your feet and calves. Stretching your calves and plantar fascia is the most effective way to relieve the pain that comes with this condition.

Surgical Treatment
Foot surgery is difficult, especially when large amounts of deformity correction are needed. The ability to bring the foot into a new position may not be lasting, even if everything looks perfect in the operating room. The goal is to provide improved position and function of the foot and ankle. In some patients with very severe deformity, the goal is a foot that functions well in a brace. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Particular complications associated with cavus foot surgery include incomplete correction of deformity, return of deformity and incomplete fusion.
Prevention
So how do you prevent plantar fasciitis? Factors which can be controlled include training progression, environmental factors, shoes, and strength and flexibility exercises. A useful guideline for a safe training progression is ?the 10% rule.? Limit increases in distance or intensity to 10% a week. For example, if a person is running 60 minutes at a session, 4 times a week, or 240 minutes, she or he can probably increase the running time to 264 minutes (240 + 10%), the following week if all else remains the same. Terrain is also an important factor in training. Running 30 minutes on hills is very different from running 30 minutes on flat surfaces in terms of the forces on the legs and feet. Work up gradually to increase your running time on hills. Also lean forward when running downhill. If you run on a banked or crowned surface, vary the direction you run in so you alternate which leg is higher and which leg is lower on the bank. If you know concrete or asphalt is causing you discomfort, try running on a cinder or composite track. If you are going on vacation and are not used to running on sand or grass, don?t spend your whole vacation doing it.